The Mysterious Case of “Lipstick Boy”
0On October 2nd 1997, a son and a father set off to make a familial visit to relatives in the Lake District. That was the last time that these two were seen alive. Their bodies were found on October 18th, two weeks after their initial disappearance. After extensive searching, John Lee (52) and Connor (14) were located at the scene of a car crash in difficult terrain near Windermere. The deaths were treated as a tragic accident, which was devastating for the family.
During the post-mortem examinations, something truly intriguing and mysterious turned up to baffle the investigators working on the case. The analysis revealed that fresh traces of lipstick had been found on Connor Lee’s lips. An article from the BBC archives states “Forensic testing indicated that the lipstick, a brand popular with pre-teens, had been applied 10-14 days after the car accident”.
The mystery naturally lies in the manner in which the lipstick came to be on Lee’s mouth. One wonders if there may perhaps be a somewhat necrophiliac side to this case. Tomas Mankovsky created a beautifully eerie short film inspired by and exploring the case.
More on the film can be read about here.
Haemolacria
0Cases of people crying blood have been reported since the 1500s, a rare disorder which we now call haemolacria- quite literally, “bloody tears”. As suspected, the condition results in tears that are partially or entirely composed of blood. Although this affliction has yet to be fully understood, there are some things that we do know.
First of all, hormonal changes can contribute. In the 16th century, some of the oldest recorded cases are Italian doctor Antonio Brassavola’s statements speaking of a menstruating nun who suffered, as well as a Flemish physician who wrote on a 16-year old girl “who discharged her flow throughout the eyes, as drops of bloody tears, instead of through the uterus.”
Interestingly enough, this is substantiated by modern science. A 1991 study of 125 healthy subjects found that menstruation contributed to traces of blood in tears, a phenomenon called “occult haemolacria”. According to the resulting paper, 18 percent of fertile women’s tears contain blood, whearas only 7 percent of pregnant women, 8 percent of men and no women who were post-menopause displayed signs of bloody tears. The conclusion reached by the scientists was that “Occult haemolacria in fertile women thus seems to be induced by hormones, whereas haemolacria most often is provoked by local factors (bacterial conjunctivitis, environmental damage, injuries).”
Injuries can also cause haemolacria. In March of 2013, a man of Canadian origin was walking along a beach when a poisonous snake bit him, resulting in agonizing swelling and kidney failure…in addition to the man weeping tears of blood. Doctors accredited the bloody tears to the prodigious amounts of internal bleeding brought about by the snake’s venom. In many cases of haemolacria, the blood can be attributed to various illnesses and ailments, including:
- Severe anemia
- Head injury
- A tear in the tear duct
- Tumors or vascular malformations
- Various coagulopathies, including haemophila
- Conjunctivitis
- Nosebleeds in someone who has “reversed” flow in the nasolacrimal ducts
Inflammation
0The word inflammation derives from the Latin “inflammo” meaning “to set alight”. Occurrences such as burns, infections, radiation exposure, or frostbite trigger this reaction. It is likely that you have had this happen to you. In the case of questions as to the internal maneuvers that cause inflammation, I hope to shed some light on the topic.
First, the blood vessels dilate and blood flow increases to the area of damage. The blood vessels themselves become more permeable, allowing the plasma to escape from the blood into the extracellular fluid, which culminates in the swelling of the region that is affected. Leukocytes, or white blood cells, also escape from blood vessels in the area, and release chemicals that may cause pain. Together, these changes produce classic inflammation symptoms- redness, swelling, heat, pain, and tenderness.
As the progression of the inflammation occurs, leukocytes migrate in expanded numbers from the bloodstream and into the area that is injured. This response continues until the invading organisms and dead tissues have been removed. Next, the inflammation is resolved-the excess fluid is drained from the region by the lymphatics, the blood vessels constrict and thus become less permeable, and the redness, swelling, and heat subside.
Additionally, if tissue damage has occurred, the healing process will also involve regeneration of tissue-the repeated division of surviving tissue cells to replace the damaged ones. Not all tissues can regenerate, however, such as nerve and brain cells. In addition, extensive damage may not procure regenerative results.
Occasionally, surgical intervention may be required to aid the healing process. In some cases, dead cells, tissue, and bacteria may congregate to for pus, which in turn may collect and form an abscess, which may need to be drained. If there are large areas of dead tissue, the dead tissue requires removal.
Anthropodermic Bibliopegy
0The practice of binding books in human skin, or anthropodermic bibliopegy, is an aged practice that has caught my attention as of late. Recently, a book from the Harvard University library has been revealed to have a rather more unusual binding of the aforementioned type. The 19th-century tome, entitled Des Destinees de l’Ame (or, translated, Destinies of the Soul) was found to have been covered by the skin of a female patient from a mental hospital who died of natural causes. Researchers utilized a technique called peptide mass fingerprinting (PMF) to determine that the proteins in the book were not of a more animal origin, and further tests concluded the skin as human.
Anthropodermic bibliopegy was a relatively common practice in the 1800s. It could be preformed as a curios, a memento, or as a punishment for criminals. One seminal example of the latter idea relates to notoriously infamous murdering pair William Burke and William Hare. The two men profited from a lucrative, ten-month-long career as body snatchers and sellers, offering them up to medical establishments for profit. In the end, after neighbors reported seeing a cadaver in Burke’s bed and victims were discovered in the dissection room of one Dr. Knox, Burke and Hare were arrested, tried, and found guilty for the murders of 16 poor citizens. Hare ended up agreeing to provide evidence against Burke so that he could escape prosecution. Burke wrote his confessions in 1829, before being hung and dissected on January 28th of the same year. The dissection was ordinary at the time, as the Murder Act of 1752 required all murderers to be publicly dissected as additional punishment. While this murderer’s skeleton can today be found hanging in the Edinburgh University Museum, his skin had a rather different ending. Burke’s skin was made into a small, dark brown pocketbook embossed with gold letters that read ‘BURKE’S SKIN POCKET BOOK’ and ‘EXECUTED 28 JAN 1829’. Today, it can be found at Surgeon’s Hall in Edinburgh.
One last question may remain-how was anthropodermic bibliopegy carried out, pertaining to the processes used to turn the skin into the binding of a book. Unfortunately, the tanners did not leave much behind in terms of written evidence (besides account books), however the books that have been collected to this day have a homologous feel and appearance to an ordinary leather-bound one, which suggests that the human skin was treated much as your usual other animal hides. Historically, the tanners removed any possibly discoloring blood by washing and soaking in water, and then soaked in a lime- or sometimes even urine-containing solution. The latter action’s purpose was to loosen the hair and fat on the skin. Afterwards, they were washed again and then treated with tannins and oils to prevent them from drying too quickly, before being hung out to dry. The skin was left to dry for about 7-10 days, at which the skin was soft and stretchy, and could be used for book-binding purposes.

The pocketbook made from Burke’s skin.
Penicillin Fungus Can Reproduce Sexually
0Fungi are a diverse group, from microscopic molds to large, forest-dwelling mushrooms. This article pertains to some interesting news related to the former, smaller end of the group. As I am certain you are already aware, mold tends to reproduce either asexually or sexually-and most commonly asexually, by forming spores. As of 2013, the previously thought asexually-reproducing Penicillium chrysogenum has been shown to have a sexual side as well. An international research team led by Julia Böhm and Prof. Dr. Ulrich Kück of the Chair of General and Molecular Botany at the Ruhr-Universität has displayed that the fungus mold also has a sexual cycle, i.e. two sexes. Through the sexual reproduction of P. chrysogenum, the researchers have produced fungal strains with new properties that are quite relevant biotechnologically- an example of this being high penicillin production that lacks the contaminant chrysogenin.
Penicillium chrysogenum is the original source of penicillin that is still in use today, It works by creating a carbon and nitrogen ring structure called beta-lactam, which averts the bacteria from building cell walls. This antibiotic aids the microscopic fungi in eradicating any bacteria that may try to habituate the area where the fungi grows, and is what doctors have used to fight bacterial illness since the 1940s.
Regardless of the decades that P. chrysogenum was studied, it was still believed that it only reproduced sexually. The idea held due to the convoluted nature of fungal sex, which involves many different reproductive strategies. Some navigate a mating scene populated by thousands of sexes, while others clone themselves asexually. Certain types of yeast can even switch their mating type. In the fungal world, the number of sexes depends on the species.
Fungal biologist Paul Dyer from the University of Nottingham had his suspicions about the mold’s reproductive habits. A complete sequence of its genome displayed that the fungus still carried the genes necessary for sexual reproduction. “That told us that there was perhaps sexual compatibility there,” he says. Dyer joined forces with other European universities to find the ideal conditions to encourage P. chrysogenum to have sex.
In the experiment, Dyer and his colleagues paired strains with compatible mating genes and grew them with different light and food conditions. The most effective combination was found to be a biotin-supplemented nutrient medium (in this case, an oatmeal base). After five weeks in a dark, oxygen-deprived environment, special structures called ascospores and cleistothecia were produced. These formations only occur after sexual reproduction. Genetic analysis confirmed that genes had been sexually recombined.
In addition, the researchers discovered that the sex genes control the activities of biologically relevant genes-in this case the ones responsible for penicillin production. In essence, the more sexually active fungi make more penicillin, which is quite fascinating.
Interestingly enough, P. chrysogenum is not the only the only fungi recently reclassified as reluctantly sexual. Dyer’s lab group has additionally learned that Aspergillus fumigatus, a mold typically found in leaf litter and compost heaps has a sexual side to it as well.
Either way, this fungi’s increased sexuality and resulting high penicillin production could lead to more effective antibiotics. In addition to the aforementioned lack of chrysogenin in the penicillin produced, there is the rather obvious yet still seminal premise of making more penicillin more efficiently and even lead to new antibiotics. Penicillin has been life-changing and life-saving in the field of medicine, and increasing the production and efficiency will ensure that it continues to do so.

A scanning electron microscopic image of asexual conidiospores from the penicillin producer Penicillium chrysogenum.
Works Cited
Fessenden, Marissa. “The Joy of Fungal Sex: Penicillin Mold Can Reproduce Sexually, Which Could Lead to Better Antibiotics.” Scientific American Global RSS. Scientific American, 08 Feb. 2013. Web. 09 Feb. 2015.
News Staff. “Discovery: Penicillin Fungus Can Reproduce Sexually After All.” Science 2.0. Science 2.0, 08 Jan. 2014. Web. 09 Feb. 2015.
“Press Release No.4.” Ruhr-Universität Bochum. Ruhr-Universität, 08 Jan. 2013. Web. 09 Feb. 2015.
Adderall
0Adderall. Perhaps you know someone who takes it; perhaps you take it yourself. Or maybe you are just curious, as many are, about the drug-its side effects, purposes, and place in our society.
Adderall is a phenylethylamine-class drug constituted from a mixture of amphetamine and dextroamphetamine used to treat attention deficit hyperactivity disorder (ADHD) and narcolepsy. Amphetamine and dextroamphetamine are central nervous system stimulants that affect chemicals in the brain and nerves that contribute to hyperactivity and impulse control. The actual chemical parts of this drug are four active ingredients that each make up an even 25 percent portion of the drug-dextroamphetamine saccharate, dextroamphetamine sulfate, amphetamine aspartate monchydrate, and amphetamine sulfate. In addition to the active ingredients, there are a number of inactive ingredients, however the four aforementioned amphetamine-based salts above give Adderall its results. Prescriptions are given in either 5, 10, 15, 20, 25, or 30 mg doses.
This drug was actually originally primarily used as a weight-loss remedy in the 1960’s, and at the time was known as Obetrol. Obetrol was never really popular and eventually was not profitable enough to stay on the market. Thus, in 1994, Rexar Pharmaceuticals sold the formula rights to Richwood, now known as Shire Richwood. By the time 1996 rolled around, the FDA had approved Adderall for treatment of ADHD in children. Adderall was first introduced in instant-release capsules, and later was made available in an extended-release type as well (the only difference being the amount of time in which they are released into the body).
Common side effects of the drug include:
- Nausea
- Appetite loss
- Stomach pain
- Dry mouth
- Anxiety
- Agitation
- Mood shifts
- Insomnia
- Headaches
- Dizziness/weakness
Adderall is highly addictive and has been taken recreationally, with many adolescents taking the drug as what they think of as a “safe alternative” to cocaine, which it is clearly not. Dangerous side effects of recreational Adderall use include heart arrhythmia, psychotic episodes, respiratory complications, increased aggression, toxic shock, and even death. Many college students use the stimulant-natured drug as a study aid, so that they can stay awake longer and concentrate better, which is both hazardous and illegal. Adderall is considered a gateway drug (when used recreationally) by some psychologists, due to it affecting the same areas of the brain as methamphetamine and cocaine.
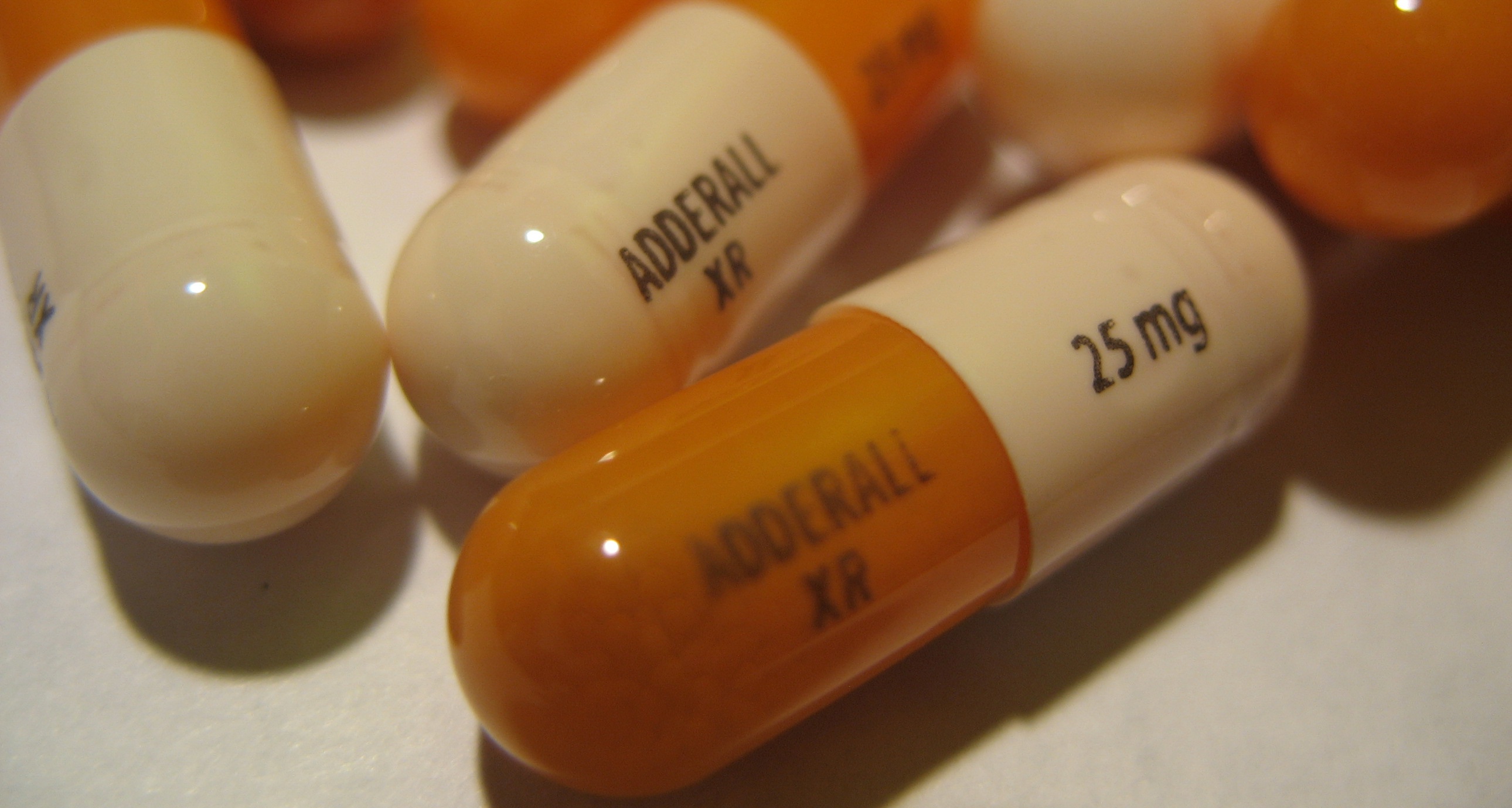
Adderall is an important drug used mainly to treat ADHD, although also as a treatment for narcolepsy. It is highly addictive and recreational usage is not recommended.
—————————————————————————————————————————————–
The Winter Solstice
0Ah, the solstice-the first official day of winter, and the start of longer days. The word deriving from the Latin words for ‘sun’ and ‘to stand still’. This year, it fell upon December 21st, and unlike some time ago, no-one was worrying about the world’s supposed end. So really, what is this event?
To begin with, it is the shortest day only for those living in the Northern Hemisphere. For those living in the south, the effect is reversed, and therefore they recently had the summer solstice. As you may already know, the tilting of the Earth and its poles towards and away from the sun causes the seasons. Up here in the North, the winter solstice is brought on by the North Pole being tilted the furthest away from the sun that it will be in the year.
The opposite is true for the summer solstice. Despite any preconceptions you may have, this date is not the coldest day of the year because the Earth still retains a great amount of thermal mass retains heat from summer and fall and the cooling process is gradual. Therefore, these coldest days generally begin about a month after the solstice. As astronomer Robert Howell put it, “If you think about turning up an oven—it takes it a long time to heat up, and after you turn it off, it takes a while for it to cool down. It’s the same with the Earth.”
So is the Solstice on the same date every year? Well, no, because the timing depends on when the Earth is tilted the furthest away from the sun. In addition, there is a discrepancy between the human calendar year of 365 days and the astronomical rotation of our blue planet, which takes about 365.24 days. Thus, the solstice is usually around the 21st of December, and not always exactly on the date. The leap year system of adding an extra day to the calendar every four years may ensure that our calendars are accurate, however it fluctuates the actual date of the solstice, making the different dates a human change and not an astronomical one.
As the writer Albert Camus once said, “In the depth of winter, I finally learned that there was in me an invincible summer.”
Hemophilia
0Hemophilia is a group of bleeding disorders. The two most common types are Hemophilia A (or classic hemophilia) and Hemophilia B (or Christmas disease).
The F8 (Factor VIII) gene produces the protein antihemophilic factor (AHF) in humans.This protein is essential for routine blood clotting functions. In individuals with hemophilia A, this protein is absent or dysfunctional. For those with the less common hemophilia B, Factor IX is the gene responsible.
Symptoms of the disorder:
- Severe nosebleeds
- Easy bruising
- Blood in urine (hematuria) /stools
- Heavy bleeding/hemorrhage after bumps, dental work, minor cuts, or other trauma
- Joint pain
- Heavy menstrual bleeding in women who are carriers
Associated Complications:
- Damage to joints (including elbows, knees, and ankles)
- Damage to muscles, causing significant scarring and pain
- Severe anemia as a result of blood loss
- Bleeding in digestive system
- Bleeding inside head (intracranial hemorrhage)
- Compartment syndrome (develops when bleeding in muscles puts pressure on the arteries and nerves within, resulting in serious limb damage)
Hemophilia is caused by a sex-linked mutation-that is, a mutation to genes that are carried on either the X or the Y chromosomes. Both types of hemophilia discussed are X-linked recessive traits.Therefore, females are usually only carriers, as they have two X chromosomes. In order for a female to have hemophilia, both of her parents must pass on the faulty genes. Males, on the other hand, have only one X chromosome, and thus if a male inherits the faulty gene, hemophilia will develop.
It is possible for a new genetic mutation to occur-that is, the person gets hemophilia even if neither parent carries a genetic mutation.
Detection of Carriers
Carriers of hemophilia are detected by a process of carrier testing. These tests may involve:
- Creating a family tree. A genetic counselor or physician may help a woman create a detailed family history called a pedigree chart in order to determine information for three generations. This chart would aid in identifying possible carriers within the family.
- Factor levels can be tested. Factor level tests, accurate 70% to 90% of the time in determining carrier status, involve the testing of the blood of the woman. On average, carriers have lower levels of factors 8 or 9 than women who are not carriers.
- DNA testing is still the most accurate method. For this test, DNA of the tested is examined for genetic changes that could cause hemophilia. The two types available are direct mutation testing, and linkage (indirect testing).
- Prenatal testing involves testing a small amount of amniotic fluid, blood from the umbilical cord or placenta, and can be done early in the pregnancy.
Treatment:
Hemophilia can be treated by injecting AHF (isolated from donated blood) into the hemophiliac (the AHF is slowly injected or dripped into the veins). The donated blood must be meticulously screened and scrutinized for infectious diseases, however the AHF injections relieve the most severe effects of the disorder. With appropriate treatment, hemophiliacs can live relatively normal lives.
Even though gene therapy remains a great hope, so far there is no workable cure for hemophilia. In a small number of hemophiliacs with liver transplants, their hemophilia was completely cured, due to the clotting factor being made in the liver. Transplants, however, are much too risky to be used as a cure.
Another possible cure is fetal hepatocyte transplantation. Fetal hepatocytes are the liver cells of an aborted fetus. These cells can function as normal liver cells would and can be grown in a laboratory. As the scientists research, they hope that these cells can eventually be placed in the body of a hemophiliac and thus produce the clotting factor for the affected person.
Some precautions to take are:
- Avoid taking nonsteriodal anti-inflammatory drugs and aspirins (these may contain blood thinners).
- Get vaccinated with the hepatitis B vaccine.
- Avoid circumcising male offspring of women known to be carriers until the infant has been tested for hemophilia.
- Carry identification information identifying those with the disorder.
- Avoid activities with a high collision risk.
- Take extra care to protect the head from injury.
- Be aware of the effects of activities with high impact.
- Practice good dental care to reduce the risk of major dental work.
So far, there are no guidelines as to how to prevent hemophilia. However, talk to genetic counselors if you have a family history of the disease so that you can calculate the risk for potential offspring.
Interesting Facts:
- Hemophilia earned the nickname “royal disease” or “disease of kings” because Queen Victoria passed on the disorder to her son Leopold who in turn passed it through many royal lineages of Europe.
- Hemophilia B is also called Christmas disease. The name originates from the first patient reported to have it, a man named Stephen Christmas.
- The disease was first called haemorrhaphilia.
Works Cited
Carson-DeWitt, Rosalyn, MD. “Hemophilia (Hemophilia A—Factor VIII Deficiency; Classic Hemophilia; Hemophilia B—Factor IX Deficiency; Christmas Disease).” Consumer Health Complete. EBSCOhost, June 2013. Web. 25 Oct. 2014.
“Complications of Hemophilia-Topic Overview.” WebMD. WebMD, 03 Aug. 2013. Web. 25 Oct. 2014.
“Gene Therapy as an Alternative to Conventional Treatment of Haemophilia.” Evoscience. Evoscience, n.d. Web. 26 Oct. 2014.
“Hemophilia Carrier Testing.” Steps for Living. NHF, 2014. Web. 25 Oct. 2014.
“Hemophilia.” KidsHealth. Ed. Suzanne Nielsen. The Nemours Foundation, 01 Jan. 2011. Web. 25 Oct. 2014.
“Hemophilia Tests.” Hemophilia Tests. RnCeus, n.d. Web. 26 Oct. 2014.
“Hemophilia.” University of Maryland Medical Center. University of Maryland Medical Center, 07 May 2013. Web. 25 Oct. 2014.
“Heredity of Hemophilia.” – Canadian Hemophilia Society. Canadian Hemophilia Society, 2014. Web. 26 Oct. 2014.
“History of Bleeding Disorders.” National Hemophilia Foundation. NHF, n.d. Web. 26 Oct. 2014.
“HoG Handbook.” Curing Hemophilia Hemophilia The Basics HoG Handbook Hemophilia of Georgia. Hemophilia of Georgia, n.d. Web. 25 Oct. 2014.
Levine, Joseph, Ph. D. “Sex-Linked Genetic Disorders.” Biology. By Kenneth R. Miller. Third ed. New Jersey: Prentice Hall, 1995. 238. Print.
“Living With Hemophilia – Bayer HealthCare.” Living With Hemophilia – Bayer HealthCare. Bayer Group, 18 June 2014. Web. 26 Oct. 2014.
Miller, Kenneth R., Ph. D., and Joseph Levine, Ph. D. Biology. Third ed. New Jersey: Prentice Hall, 1995. Print.
“National Hemophilia Foundation.” National Hemophilia Foundation. NHF, n.d. Web. 26 Oct. 2014.
“Patient Education: About Hemophilia.” UC San Diego Health System. UC San Diego Health System, 2014. Web. 25 Oct. 2014.
Shapiro, Amy D., MD, and Whitney Sealls, Ph. D. “Hemophilia B.” Rare-Diseases. National Organization for Rare Disorders, 2014. Web. 26 Oct. 2014.
“What Causes Hemophilia? :: DNA Learning Center.” DNALC Blogs. Cold Spring Harbor Laboratories, n.d. Web. 25 Oct. 2014.
“What Causes Hemophilia?” – NHLBI, NIH. NHLBI, NIH, 31 July 2013. Web. 25 Oct. 2014.
Stages of Death
2I have always been fascinated by death, related customs and the dying process. Although naturally a part of life, it is still pinpointed as taboo. For many people, myself included, it is a topic shrouded in mystery. When something is unknown to me, I often develop a curiosity about it, often leading to a passion. Such a situation led to my interest in mortuary science.
Many past cases of believed vampires were actually due to the misunderstanding of the dying process, which basically follows as such:
Post-mortem, the fastest and first step is pallor mortis, Latin for ‘paleness of death.’ This stage is most visible in those with lighter-toned skin and is caused by the lack of blood circulations in the capillaries and therefore body. Pallor mortis can begin minutes after death.
The second stage is algor mortis, or coldness of death. This describes the reduction in body temperature following death. Until ambient temperature
Livor mortis is ‘discoloration of death’ and it is a function causing usually bluish-purple discoloration of the skin due to the pooling of blood in the dependant parts of the body after death. Note that the blood will gravitationally migrate to the lowest point in the body. After about 12 hours, the lividity becomes fixed.
The next and most well-known is rigor mortis, also known as stiffness of death. This stage lasts approximately 36-72 hours (2-3 days). Rigor mortis is a chemical change (the loss of adenosine triphospahate, ATP) to the muscles in a body, causing them to stiffen up. It tends to start around the eyes and other smaller facial muscle groups and thus spreads downward to the larger muscles.
After this time period, during secondary flaccidity, the muscles relax again. This is due to the decay of your muscles, allowing them not to be as contracted as they were in rigor mortis.
Next, decomposition begins to set in. Decomposition is when organic substances (i.e. your body) are broken down into simpler forms of matter(helped along by natural decomposers, such as maggots and scavengers such as vultures). After a body begins to decompose, putrefaction begins.
Putrefaction is when bacterial enzymes cause destruction of soft tissues in the body. Essentially, the bacteria living inside your body eats its way out, resulting in things such as gas buildup, bloating, swelling, skin slip, and liquefying tissue, all leading to the final result of skeletonisation.






